Free Kidney Nephrons: Filtering the Blood revision notes for OCR A Level Biology – covering specification points 5.1.2 (ci) and 5.1.2 (ciii).
Nephrons
A nephron is a tubular structure responsible for filtering the blood and forming urine.
The nephron consists of a number of structures that work together. Their arrangement with respect to each other, a dense capillary network, and their position in the kidney set up concentration gradients for the effective filtration and reabsorption of substances.
The diagram below shows the structures of a single nephron and their relative positions in the kidney tissues:
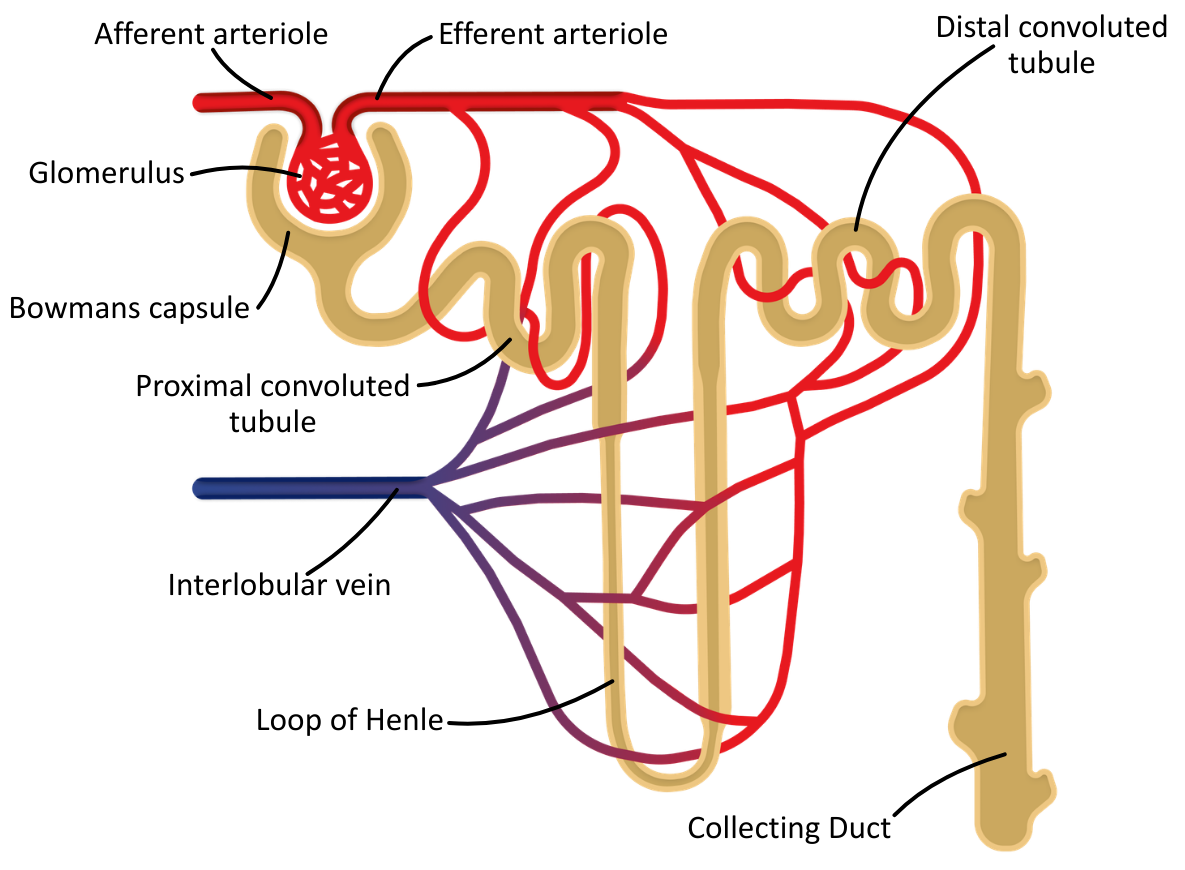
It is important to note that the collecting duct is not a component of the nephron; however, in A level materials, it is usually referred to as such, and for simplicity, it will be included with the nephron.
Blood Filtration: The Nephron
The nephron’s structures are adapted for their own function; together, they can filter blood and reabsorb substances in the needed quantities.
The table below outlines the function of each structure:
| Nephron Structure | Function |
|---|---|
| Bowman’s capsule and glomerulus | Ultrafiltration: Filtration of small molecules from the blood plasma under pressure. |
| Proximal convoluted tubule (PCT) | Selective reabsorption: Recovery of useful solutes and most of the water. |
| Loop of Henle | Creation of a steep osmotic gradient. |
| Distal convoluted tubule (DCT) | Homeostatic balancing of ions and pH. |
| Collecting duct | Osmoregulatory water reabsorption in response to ADH. |
Ultrafiltration
Ultrafiltration takes place in the renal corpuscle and is the first stage of blood filtration, leading to urine production.
Blood enters the glomerulus from the afferent arteriole, which is larger than the exiting efferent arteriole. This creates a higher hydrostatic pressure in the knot of capillaries than in the surrounding Bowman’s capsule, forcing out water and solutes from the blood, which form the glomerular filtrate.
Glomerular filtrate is essentially blood plasma without large proteins or cells, consisting of:
- Water
- Glucose
- Amino acids
- Urea
- Ions (Na⁺, Cl⁻, K⁺, HCO₃⁻)
The blood plasma leaving the glomerulus (via the efferent arteriole) has a low (negative) water potential, which is essential for reabsorption later in the nephron.
Red and white blood cells, and plasma proteins, remain in the blood because they are too large to cross the filtration barrier into the Bowman’s capsule.
The diagram below shows the structure of the filtration barrier:

The table below outlines the structures of the filtration barrier:
| Filtration Barrier Structure | Description |
|---|---|
| Capillary endothelium | Single layer of cells lining the glomerular capillaries, with small pores called fenestrations. |
| Basement membrane | Collagen and glycoprotein mesh* located between the capillary and podocyte layers. |
| Podocyte layer | Epithelial cells (of the Bowman’s capsule) form narrow filtration slits with membrane extensions, called major processes, which have smaller extensions called minor processes. |
*Molecules with a relative molecular mass larger than69,000 are unable to pass through the mesh of the basement membrane, such as albumin, antibodies, and fibrinogen.
Selective Reabsorption (in the PCT)
Selective reabsorption takes place in the proximal convoluted tubule (PCT), and is the second stage of blood filtration in the kidneys.
Selective reabsorption is the process by which useful substances from the glomerular filtrate are reabsorbed back into the blood through both active transport and (passive) co-transport mechanisms.
The table below outlines the key substances selectively reabsorbed from the filtrate in the PCT:
| Substance | Mechanism of Reabsorption |
|---|---|
| Amino acids | Co-transported with Na+ ions into epithelial cells, then diffuse into capillaries. |
| Cl– | Follow Na+ diffusion down an electrochemical gradient. |
| Glucose | Co-transported with Na+ ions into epithelial cells, then diffuse into capillaries. |
| Na+ | Actively transported out of epithelial cells into the tissue fluid/blood via Na+/K+ ATPase pumps. |
| Small proteins and peptides | Reabsorbed by endocytosis into epithelial cells. |
| Water | Diffuses down the water potential gradient (osmosis) established by solute reabsorption. |
Mechanism of Selective Reabsorption
- Sodium–potassium pumps on the epithelial cell surface membrane actively transport Na⁺ ions out into the surrounding tissue fluid.
- Sodium ions diffuse in from the filtrate in the PCT into the epithelial cells down a concentration gradient. Glucose or amino acids are moved with Na⁺ through co-transport proteins.
- Water moves out of the PCT and into the epithelial cells by osmosis down the water potential gradient.
- Na⁺ are actively transported out of the epithelial cells into the blood of the capillary.
- Water diffuses down the water potential gradient established by the movement of Na⁺ into the blood of the capillary by osmosis.
- Amino acids and glucose diffuse into the bloodstream down the concentration gradient maintained by the capillary network.
The PCT reabsorbs nearly all glucose and amino acids, and around 85% of water and sodium ions from the filtrate.
The Hairpin Countercurrent Multiplier System
The hairpin countercurrent multiplier system is a process arising from the structure and function of the Loop of Henle.
The Loop of Henle works to create a steep osmotic gradient in the medulla of the kidney, so that water will move out of the loop of Henle (and later the collecting duct) as it passes through the nephron, being reabsorbed back into the blood.
The diagram below shows the structure of the Loop of Henle and the movement of substances:
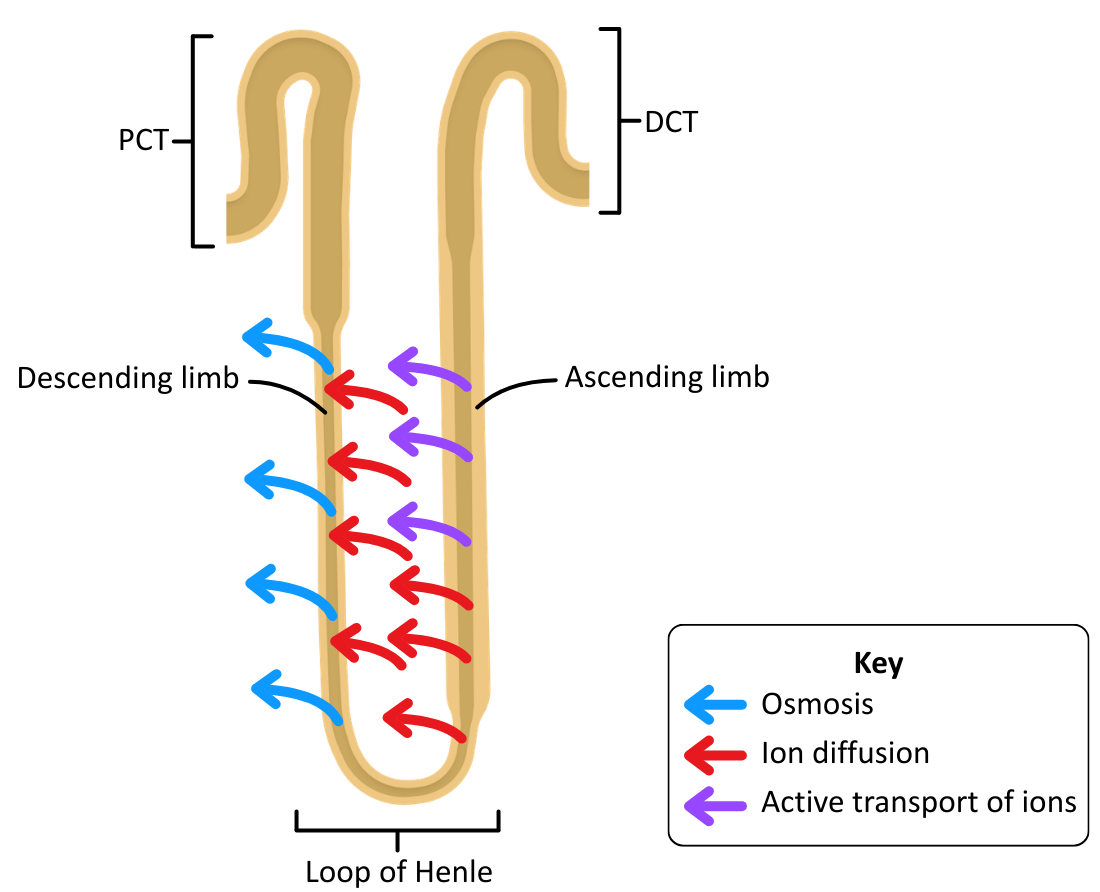
The descending limb is permeable to water, but the ascending limb is not.
Mechanism of the Hairpin Countercurrent Multiplier System
- Water moves out of the descending limb by osmosis into the medulla because the water potential is lower.
- Sodium and chloride ions diffuse into the descending limb from the medulla, down their concentration gradient.
- Sodium and chloride ions diffuse out of the lower ascending limb into the medulla.
- Sodium and chloride ions are actively transported out of the upper ascending limb into the medulla, further lowering the water potential of the medulla.
- Water remains in the filtrate because the ascending limb is impermeable to water, so the filtrate becomes more dilute as ions are transported out.
- The accumulation of sodium and chloride ions in the medulla establishes a steep water potential gradient from the cortex down to the base of the medulla, allowing water to be reabsorbed later from the collecting duct by osmosis.
When the filtrate reaches the top of the ascending limb, and the end of the loop of Henle, its water potential has increased (become less negative) as most sodium and chloride ions have been removed into the medulla.
Selective Reabsorption (in the DCT)
In OCR A Level Biology the distal convoluted tubule’s role in blood filtration is often skimmed over.
The distal convoluted tubule (DCT) is located in the cortex, and is the final section of the nephron (because the collecting duct is not actually a part of the nephron), connecting the ascending limb of the loop of Henle to the collecting duct.
The DCT adjusts the composition of the filtrate by selectively reabsorbing ions and secreting hydrogen or potassium ions to regulate pH and electrolyte balance in the blood.




